Psoriatic arthritis (PsA) is a kind of arthritis seen in people with Psoriasis. It’s an inflammation-related condition that causes stiffness, joint pain, and swelling.
The majority of people experience psoriasis-related symptoms on their skin before they show symptoms of PsA; however, some people begin to notice signs of arthritis first.
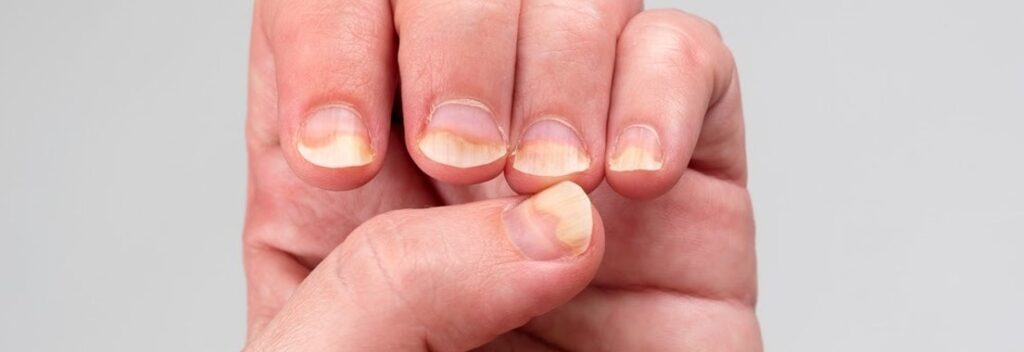
Patients with PsA frequently experience signs that affect their nails. Indeed, Psoriasis of the fingernails is often an indicator of PSA. According to a review of research Trusted Source published in 2017, approximately 80 percent of those who suffer from PsA have nail lesions.
Find out more about the ways PsA can alter your nails.
Sights and signals
Psa can trigger a variety of nail problems. Be aware that not all people who suffer from PsA suffer from these issues, while others might experience just one or two nail issues.
Pitting
Many people suffering from PsA suffer from nail psoriasis that can cause pitting. This can cause your nails to appear as if they have tiny holes or dents. They may be rough or bumpy on the surface.
Pitting occurs when an unusual cell growth results in the formation of nail deposits. If these deposits are removed, they create holes and scratches.
The nail continues to expand around these areas.
Separation
PSA may cause the nail to split from the nail bed. It can happen in tiny pockets or throughout your pin. If a small portion of your nail rises off the nail bed, it could appear as the appearance of a white or clear area.
Nail separation is caused by inflammation of the nail’s nail bed.
The white spots
Psa can result in white patches on your nails. They usually occur at the centre of the nail.
They signify that you may have psoriatic lesions on your nail matrix. This is the portion that forms the bed of your nail in which new nail cells are created.
Discoloration
For sure, PsA can cause nail discoloration. The result could cause your nails to appear oil-stained. The exact colour of these stains can differ, but they usually are either purple or pink shade.
They’re caused by the accumulation of cellular debris underneath the nail.
The red spots
Another indication of PsA is the white half-moon near the nail’s root, also known as the lunula. A few people who suffer from PsA are prone to red spots within this area, but nobody knows what causes them. These spots could indicate the formation of blood vessels that are not yet formed.
Flaking or cratering
People suffering from PsA might have nails that look to be:
- Crinkling up
- crumbling
- peeling off layers of flake
The flaking and sagging of your nails can occur due to irritation or the presence of excess skin cells that are in the nail bed.
Ridges
People who suffer from PsA may have vertical ridges that run and down the nails. They look and feel similar to raised lines.
They are caused by psoriatic lesions that appear within the matrix of nails.
Purple spots that split with nails
The splitting process is usually carried out together with lines. The nail could split vertically on any of these ridges.
If you notice a dark spot in the ridge, this could indicate bleeding that is splitting. They occur when blood vessels rupture and let blood leak into minor fractures in the nail.
Infections
Fraying and cracking can make your nails susceptible to infection by mold and bacteria. This can cause the condition known as paronychia (a state of the pin) or nail fungus.
What is the PSA-related nail problems addressed?
Nail issues caused by PsA generally respond well to standard PsA treatments, including oral medications that minimize inflammation while protecting joints from injury.
Common medicines used for PsA comprise:
- Nonsteroidal anti-inflammatory medicines (NSAIDs). NSAIDs aid in reducing inflammation and treating simple. This medication category comprises ibuprofen (Advil, Motrin) and naproxen (Aleve).
- Drugs that modify the course of rheumatic disease (DMARDs). DMARDs include methotrexate as well as leflunomide , Apremilast , and Sulfasalazine help to keep PsA from permanently damaging joints.
- Biologic drugs. Biologics are a modern generation of arthritis medications created by genetic engineering. They are designed to reduce inflammation in the body.
Specific treatments specifically target your nails. Some therapies target your nails directly, for example:
- Injections of cortisone. Cortisone injections usually focus on inflammation within a single joint. Still, they may also be injections in the nail bed to decrease inflammation and fight psoriatic lesions.
- Steroid cream. Your doctor can prescribe a steroid lotion for you to apply directly to your nails.
- Therapy with light. Light therapy (phototherapy) uses UV light to treat the psoriasis process by slowing down skin cell development. It can be done at home, using special equipment, or in the office of your doctor to treat nail psoriasis.
- Antifungal medications. If you develop a fungal nail infection, your doctor might prescribe a topical antifungal cream.
- Antibiotics. If you have an infection with bacteria on your nail, you might need oral antibiotics.

Home solutions in PsA
A few home remedies can reduce the symptoms of PsA on nails. There are a few things you can do to combat nail psoriasis.
- Make sure your fingernails are clean and neatly cut.
- Make sure your feet and hands are moisturized with a fragrance-free light lotion.
- Use gloves when performing household chores or manual labor like washing dishes.
- Beware of soaking your hands and feet in boiling water. It could cause dryness.
- Use a nail brush with a soft bristle in place of sharp items for cleaning the nail.
- Do not pick or bite your nails or the skin around them.
- Take care to treat hangnails properly and apply an antibiotic ointment if required.
- Make sure that manicures and pedicures are performed in unsanitary conditions.
- Do not wear artificial nails.
Be sure to inform your doctor about any natural or herbal remedy like turmeric, which can help reduce inflammation. The effectiveness of natural remedies has not been established.
When should you see a doctor?
Psoriasis of the nails could be an early indicator of PsA, the condition that causes inflammation which can cause other problems with the pins.
Although some of these problems are inevitable, paying attention to your nails and safeguarding them from infection may lower the risk.
If you notice any indications of Psoriasis, or any fungal infection, consult your doctor. If you have Psoriasis and you see new nail signs, the doctor will determine the cause and treat the area.
Finding the appropriate treatment and relief from symptoms is a lengthy process. But new therapies are being studied every day, which could provide relief.

