Osteoarthritis (O.A.) can be an arthritis type that is common which is most often related to knees. In the beginning, the patient may not experience any symptoms. However, in later stages, they might be afflicted with mobility issues and require a surgical procedure.
O.R. in the knee can affect the knee joint’s cartilage, bones, and synovium.
Cartilage is a slick tissue that offers a soft surface that allows joint movement and serves as a buffer between bones. Synovium, which is soft tissue and runs along joints, creates a synovial fluid that lubricates joints and supplies oxygen and nutrients to cartilage.
When these functions cease, and the body’s defences are no longer effective, they do not secure the knee bones. Joint. This can cause bone damage.
osteoarthritis that affects the knee may cause stiffness and pain. The symptoms can get worse over time.
Stages
OA that affects the knee can take some time to become a reality. Doctors typically employ stages to explain the development.
They commonly use the Kellgren-Lawrence (K.L.) classification rested Source of O.A. to describe O.A. of the knee, but other grading systems exist. The first K.L. classification was released in 1957.
The following stages follow the K.L. classification, which is based on an array of X-ray images of O.A. of the knee.
Stage 1: Minor
A scan may not reveal any injury, but bony bone growths known as osteophytes could be an early indication of osteoarthritis.
Other joint changes at this time could be minor damage to cartilage and a shrinking of the space between the bones of the joint.
At this point, the patient is likely to feel discomfort or discomfort. The joint should appear suitable on an X-ray. Gait-related changes are likely to occur.
Stage 2: Mild
At this point, the X-ray may reveal a narrowing of the joint space between the joint and bones spurs.
One may begin to feel stiffness or joint discomfort after having a break for a time.
The bone-bone junction joined with the tissues begin to become rigid. However the bone gets denser and thicker as the tissues become more brutal. The bone’s thin layers can be formed beneath the cartilage that forms in joints.
There could be a small number of injuries, but the bones are not scraping or rubbing against one another. Synovial fluid exists and helps to decrease friction, assisting the knee’s movement.
Stage 3: Moderate
At this point, the X-rays will reveal:
- a noticeable narrowing of the joint space
- the development of bone spurs
- specific damage to cartilage and other tissues
- an occurrence of a deformity that could occur on the ends of the bones
Someone may observe:
- discomfort or pain from daily exercises, like running or walking, kneeling and the bending
- Early signs for arthritis
- The swelling and buildup of fluid around the joint result from synovitis, which some people refer to as water on the knee.
As osteoarthritis advances, it will cause the cartilage to shrink and eventually fall apart. The bones react by thickening and then forming bony outward-facing growths.
Stage 4: Severe
At this point, an X-ray can show:
- A severe reduction in joint space due to where the bones meet and rub
- Significant growth of bone spurs
- evident cartilage damage, which could have become ultimately or nearly completely eroded
- A distinct deformity is seen at the end of the bone
People may experience:
- stiffness of the joint
- persistent inflammation
- less fluid in the joint.
- More friction, more friction
- severe pain and discomfort when performing simple motions
At this point, the doctor might recommend surgery.
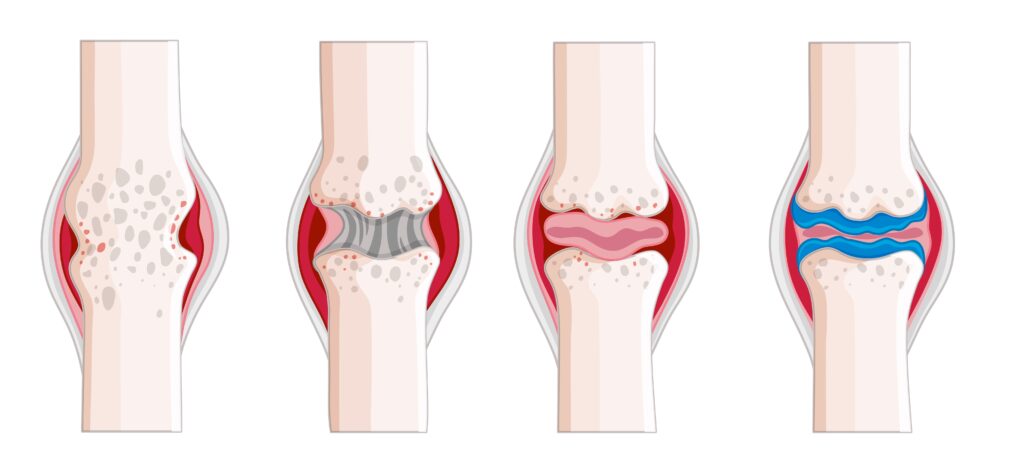
Diagnosis of osteoarthritis
One may not notice symptoms until the beginning stage of osteoarthritis.
If someone is experiencing an injury to the knee, a physician will examine the signs, including:
- the time and place that when and where
- whether the knee pops or cracks when you move it
- the duration of any pain during the morning
- how this impacts their daily day
- for instance, if they’re on any medication
- If there is pain and swelling behind the knee, it could mean the presence of the knee is affected by a Baker’s cyst is present.
- if the knee seems unstable
- within the last year, whether it has altered the joint in the shape
- Regardless of whether the symptoms are affecting either knee or both knees.
The pain from osteoarthritis in the knee generally is relieved within thirty minutes after waking up from a rest; however, the discomfort caused by Rheumatoid Arthritis (R.A.) may last more than 45 minutes.
The doctor may also:
- inquire about family and personal medical history
- Perform a complete physical exam
- Place an order for diagnostic tests
The doctor will assess the joints, measure their range of motion and look for signs of injuries. However they may focus on any areas that are painful, tender or swelling.
Tests that could be performed may include:
- X-rays are used to determine the extent of any joint damage
- MRI scans can help identify the first signs that an X-ray might not detect.
- Tests for blood to identify other conditions like Gout and RAS.
In certain instances, the doctor might recommend a joint fluid analysis that involves the removal of some fluid by needle and then sending it off to a lab to test. The results could reveal biomarkers of inflammation.
However, experts advise against this procedure unless there is swelling, which could be a sign of synovitis or joint inflammation. In this scenario, tests can help identify R.A.
Treatment of osteoarthritis
Treatment options are based on the severity of osteoarthritis and the speed at which the condition is getting worse.
Stage 1
The majority of symptoms are minor, And acetaminophens and other prescription (OTC) drugs can usually help relieve discomfort. The doctor might recommend specific exercises to improve mobility and strength.
As per the American Academy of Orthopaedic Surgeons (AAOS), there isn’t enough evidence to prove that supplements like glucosamine aid.
Stage 2
Treatments may consist of:
- taking medication for pain
- attending physical therapy sessions to increase or keep flexibility and strength
- wearing a knee brace made to alleviate pressure on joint’s surfaces
- using shoe inserts to lessen the strain on the knee.
At this point, it is possible to alter or modify routine activities to prevent discomfort.
Stage 3
Treatments may consist of:
- Utilizing OTC painkillers, like Acetaminophen
- using prescription painkillers, for example, oxycodone as well as codeine
- receiving corticosteroid injections
The past was when many were using hyaluronic acid to relieve pain. However, both the American College of Rheumatology (ACR) and the Arthritis Foundation (A.F.)Trusted Source caution against using this method, as there isn’t enough evidence to suggest safe or effective.
Stage 4
At this point, the cartilage has drastically diminished or completely lost.
The person may keep taking medications for pain relief. A walker, cane or brace may help remain mobile.
A physician may suggest an operation to repair or replace the joint.
Alternative remedies for osteoarthritis
The ACR and the A.F. suggest trusted Sources that can be used by a person who:
- achieve a moderate weight depending on the situation.
- find out information about how to handle their situation
- practice tai chi
- Use a knee brace
- Do balance exercises
- practice yoga
- take Cognitive Behavioral Therapy to relieve mood, pain, and sleep issues.
The people can try:
- acupuncture
- Magnetic pulse therapy
- needle lavage, which entails inserting a needle in the joint and then injecting a solution of saline
However, the AAO states that there isn’t enough evidence to prove that these treatments are safe and efficient.
The current guidelines by Trusted Source recommend against wedges for medial or lateral wedges shoes, supplements with glucosamine or chondroitin supplements since studies have not proved that they are effective.
Stem therapy with cells
Researchers are investigating whether stem cells therapy could help regenerate cartilage for people suffering from osteoarthritis
However, there is some obstaclesTrusted Source are facing. For example, the treatment is costly; one might need to go through many rounds before seeing results. The treatment could not be effective if the BMI exceeds 35.
The authors of the meta-analysis from 2018 examined using stem cells for treating O.A. and the impact this had on the long-term outcomes. They concluded that their findings of studies with high-quality research did not match.
Some clinics offer stem cells treatment for O.A. However, they are not recommended by the Food and Drug Administration (FDA). Trusted Source advised people of 2017 to not “believe the hype.”
The ACR and AFTrusted Source strongly discourage using stem cell therapy since there is no standard for regulating this practice.
The adverse effects of unapproved stem cell treatments could include:
- adverse reactions that occur at the site of the injection
- cells that reproduce in the wrong place
- cell’s inability to perform in the way that is expected
- an increased possibility of cancer
Anyone thinking about stem cell treatment to treat osteoarthritis should consult a physician first.
Summary
The knee joint O.A. is a chronic condition that causes cartilage to break down within the bones joints.
As time passes, bones will begin to rub, and bone spurs could form. There will be a rise in levels of stiffness and pain and possibly a decrease in mobility.
Many treatment options can be used to manage O.A. A physician will suggest treatments based on the personal needs and the severity of osteoarthritis the patient has.

